A nice article by Prof. Karl Linden at U Colorado, republished from “The Conversation” under CC license. Prof. Linden is a well-known fellow member of the UV research community and IUVA organization. I couldn’t say it any better than him!

Karl Linden, University of Colorado Boulder
Ultraviolet light has a long history as a disinfectant and the SARS-CoV-2 virus, which causes COVID-19, is readily rendered harmless by UV light. The question is how best to harness UV light to fight the spread of the virus and protect human health as people work, study, and shop indoors.
The virus spreads in several ways. The main route of transmission is through person-to-person contact via aerosols and droplets emitted when an infected person breathes, talks, sings or coughs. The virus can also be transmitted when people touch their faces shortly after touching surfaces that have been contaminated by infected individuals. This is of particular concern in health-care settings, retail spaces where people frequently touch counters and merchandise, and in buses, trains and planes.
As an environmental engineer who studies UV light, I’ve observed that UV can be used to reduce the risk of transmission through both routes. UV lights can be components of mobile machines, whether robotic or human-controlled, that disinfect surfaces. They can also be incorporated in heating, ventilating, and air-conditioning systems or otherwise positioned within airflows to disinfect indoor air. However, UV portals that are meant to disinfect people as they enter indoor spaces are likely ineffective and potentially hazardous.
What is ultraviolet light?
Electromagnetic radiation, which includes radio waves, visible light and X-rays, is measured in nanometers, or millionths of a millimeter. UV irradiation consists of wavelengths between 100 and 400 nanometers, which lies just beyond the violet portion of the visible light spectrum and are invisible to the human eye. UV is divided into the UV-A, UV-B and UV-C regions, which are 315-400 nanometers, 280-315 nanometers and 200-280 nanometers, respectively.
The ozone layer in the atmosphere filters out UV wavelengths below 300 nanometers, which blocks UV-C from the sun before it reaches Earth’s surface. I think of UV-A as the suntanning range and UV-B as the sun-burning range. High enough doses of UV-B can cause skin lesions and skin cancer.
UV-C contains the most effective wavelengths for killing pathogens. UV-C is also hazardous to the eyes and skin. Artificial UV light sources designed for disinfection emit light within the UV-C range or a broad spectrum that includes UV-C.
How UV kills pathogens
UV photons between 200 and 300 nanometers are absorbed fairly efficiently by the nucleic acids that make up DNA and RNA, and photons below 240 nanometers are also well absorbed by proteins. These essential biomolecules are damaged by the absorbed energy, rendering the genetic material inside a virus particle or microorganism unable to replicate or cause an infection, inactivating the pathogen.
It typically takes a very low dose of UV light in this germicidal range to inactivate a pathogen. The UV dose is determined by the intensity of the light source and duration of exposure. For a given required dose, higher intensity sources require shorter exposure times, while lower intensity sources require longer exposure times.
Putting UV to work
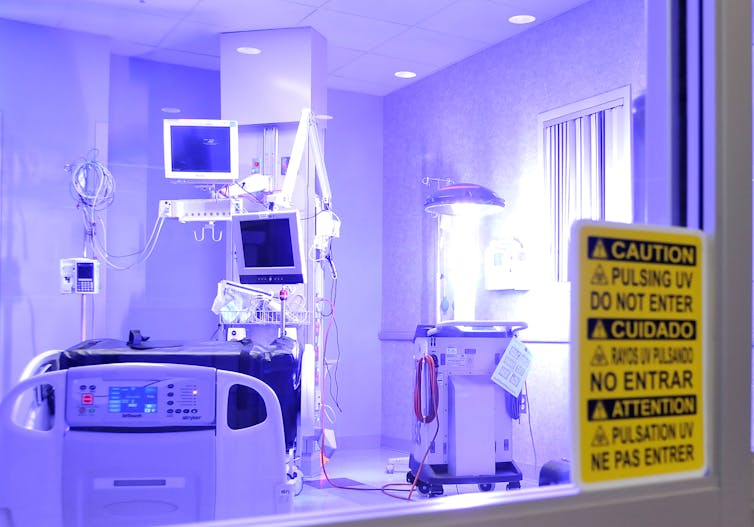
There is an established market for UV disinfection devices. Hospitals have been using robots that emit UV-C light for years to disinfect patient rooms, operating rooms and other areas where bacterial infection can spread. These robots, which include Tru-D and Xenex, enter empty rooms between patients and roam around remotely emitting high-power UV irradiation to disinfect surfaces. UV light is also used to disinfect medical instruments in special UV exposure boxes.
UV is being used or tested for disinfecting buses, trains and planes. After use, UV robots or human-controlled machines designed to fit in vehicles or planes move through and disinfect surfaces that the light can reach. Businesses are also considering the technology for disinfecting warehouses and retail spaces.

It’s also possible to use UV to disinfect air. Indoor spaces like schools, restaurants and shops that have some air flow can install UV-C lamps overhead and aimed at the ceiling to disinfect the air as it circulates. Similarly, HVAC systems can contain UV light sources to disinfect air as it travels through duct work. Airlines could also use UV technology for disinfecting air in planes, or use UV lights in bathrooms between uses.
Far UV-C – safe for humans?
Imagine if everyone could walk around continuously surrounded by UV-C light. It would kill any aerosolized virus that entered the UV zone around you or that exited your nose or mouth if you were infected and shedding the virus. The light would also disinfect your skin before your hand touched your face. This scenario might be possible technologically some day soon, but the health risks are a significant concern.
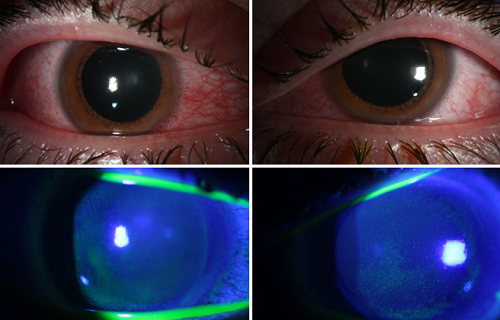
As UV wavelength decreases, the ability of the photons to penetrate into the skin decreases. These shorter-wavelength photons get absorbed in the top skin layer, which minimizes DNA damage to the actively dividing skin cells below. At wavelengths below 225 nanometers – the Far UV-C region – UV appears to be safe for skin exposure at doses below the exposure levels defined by the International Committee on non-Ionizing Radiation Protection.
Research is confirming these numbers using mouse models. However, less is known about exposure to eyes and injured skin at these Far UV-C wavelengths and people should avoid direct exposure above safe limits. https://www.youtube.com/embed/YATYsgi3e5A?wmode=transparent&start=0 Research suggests that far UV-C light might be able to kill pathogens without harming human health.
The promise of Far UV-C for safely disinfecting pathogens opens up many possibilities for UV applications. It’s also led to some premature and potentially risky uses.
Some businesses are installing UV portals that irradiate people as they walk through. While this device may not cause much harm or skin damage in the few seconds walking through the portal, the low dose delivered and potential to disinfect clothing would also likely not be effective for stemming any virus transmission.
[Deep knowledge, daily. Sign up for The Conversation’s newsletter.]
Most importantly, eye safety and long-term exposure have not been well studied, and these types of devices need to be regulated and validated for effectiveness before being used in public settings. The impact of continuous germicidal irradiation exposure on the overall environmental microbiome also needs to be understood.
As more studies on Far UV-C bear out that exposure to human skin is not dangerous and if studies on eye exposure show no harm, it is possible that validated Far UV-C light systems installed in public places could support attempts at controlling virus transmission for SARS-CoV-2 and other potential airborne viral pathogens, today and into the future.
Karl Linden, Professor of Environmental Engineering and the Mortenson Professor in Sustainable Development, University of Colorado Boulder
This article is republished from The Conversation under a Creative Commons license. Read the original article.